|
LARYNGOTRACHEAL OBSTRUCTION (CHAO = CONGENITAL
HIGH AIRWAY OBSTRUCTION) |
(Laryngeal atresia and webs, subglottic stenosis and high tracheal atresia and stenosis).
Congenital laryngeal or tracheal atresia is a rare malformation almost always incompatible with life. The level of obstruction may be subglottic (laryngeal), proximal or distal tracheal. The site of obstruction may be determined antenatally (1) and may be important, as infants with subglottic atresias have survived by performing an emergency tracheostomy (2). Congenital anomalies of the trachea usually have associated esophageal anomalies (depending on the timing of the derangement) as in the embryo the esophagus and respiratory tract have a common origin from the anterior foregut.
The etiology is unknown, although sporadic, genetic (3) and vascular causes (4) have all been proposed.
REPORTED CASES |
Link to Table of Reported Cases
ULTRASOUND |
Antenatal diagnosis is possible because of the secondary structural changes that are present in the fetal lung as a result of the laryngeal atresia.
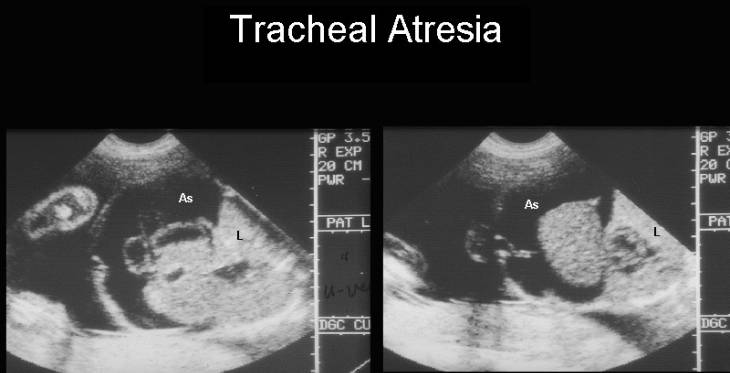
- Bilateral symmetrically enlarged hyperechogenic lungs. Upper airway obstruction promotes pulmonary hyperplasia (5) causing over-distention of the alveoli by lung fluid (6), resulting in numerous tissue-filled spaces, which reflect far more echoes than the normal lung producing the characteristic hyperechogenic appearance antenatally.
- Echogenic lungs increase chest circumference and may compress the heart.
- The majority of tracheal atresias are associated with an esophageal fistula with normal appearing lungs as the pulmonary fluid can escape into the gastrointestinal tract.
- Ascites (the hyperplastic and distended lungs invert the diaphragm, compress the heart and impair venous return to the right atrium).
- Polyhydramnios (as a result of either obstruction of the esophageal passage of amniotic fluid by the enlarging lung mass or compression of the stomach and intestines by the fetal ascites).
- +/- Fetal hydrops.
- Color doppler
- Normal fluid flow in the upper trachea can be demonstrated during fetal breathing activity. Opening of the glottis can be seen during fetal breathing.
- In CHAO there is absence
of fluid flow during rhythmic thoracic movements.
|
|
|
|
Video clip of Tracheal Atresia
|
|
|
|
|
|
ASSOCIATED SYNDROMES |
·
Fraser
syndrome (7,8).
·
VATER association (9).
·
DiGeorge developmental field defect (10).
·
Rhizomelic
chondrodysplasia punctata (11).
DIFFERENTIAL DIAGNOSIS |
The differential diagnosis of enlarged echogenic lungs includes type III
cystic adenomatoid malformation (12), pulmonary sequestration, diaphragmatic
hernia and mediastinal teratoma. However with the exception of a small
percentage of cases with type III cystic adenomatoid malformation the other
lesions are almost always unilateral whereas laryngeal atresia always produces
bilateral echogenic lungs.
REFERENCES |